The Struggles And Strengths Of Mothers Raising Children With Special Needs
In resource-restricted countries like Nigeria, parents of children with neurological disorders bear the entire burden of care.
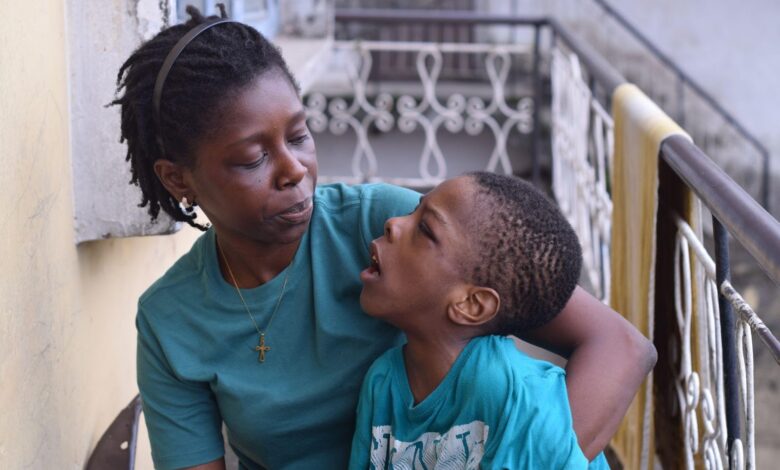
In an unexpected turn of events in early 2015, Modupe Famodun received her son’s cerebral palsy diagnosis.
A neurologist at the Federal Neuropsychiatry Hospital (FNPH) in Lagos, South West Nigeria, had been strolling down the hospital corridor when an unusual shrill cry pierced the air, immediately drawing her attention. Her instinct, sharpened by years of experience, led her to believe something was wrong.
Upon inquiry, she found out that the crying child was Tiolu, Famodun’s then two-month-old son.
Filled with empathy for the young mother, the neurologist rallied a team within the hospital to conduct a series of laboratory tests for little Tiolu. She had done all of this without any charge.
“What is cerebral palsy?” Famodun recalled asking the neurologist after she disclosed the test result. Cerebral palsy is the medical term for a group of disorders that affect a person’s ability to move and maintain balance and posture and now her son Tiolu has been diagnosed with it.
Unable to come to terms with her son’s cerebral palsy diagnosis, Famodun repeated the test at the Lagos University Teaching Hospital two months later.
She was desperate for a different outcome, but reality soon hit her. The result was no different from the first.
“This was the moment that brought me to tears because I was completely unprepared,” she said, her voice quivering as she fought her emotions.
In resource-restricted countries like Nigeria, parents of children with neurological disorders bear the entire burden of care. A study by Andrew Olagunju, a Nigerian psychiatrist and researcher, and his colleague noted that such parents are predisposed to psychological stress. The impact is even more profound on mothers, who assume greater caregiving responsibilities.
In the following months, she would grapple with overwhelming anxiety as she contemplated the chances of her son ever living a normal life.
“I shut myself in and cried endlessly, hoping on God for a miracle,” she shared.
During the initial two months of her self-imposed isolation, she could barely bring herself to touch her son except when she needed to breastfeed him. Her husband took on all the duties.
“I was lost, totally lost,” she admitted.
She still harboured guilt for Tiolu’s condition, blaming herself for the events surrounding his early days.
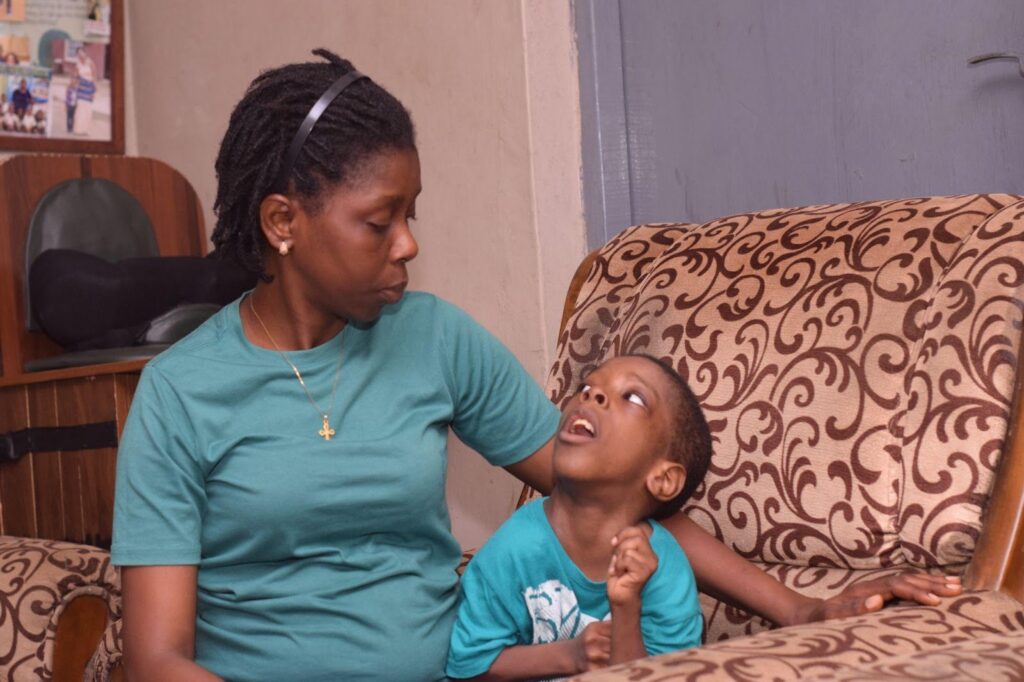
Three days after Tiolu’s birth in 2014, Famodun suspected he had jaundice, but a senior family member played down her fears. By the fifth day, when she finally sought medical help, it was already too late. In fact, he was presumed dead at the hospital. Eventually, the doctor resuscitated him but hinted at possible brain damage.
The medical confirmation of Tiolu’s cerebral palsy brought back those painful moments from 2014. She wrestled with regrets, guilt, and sorrow all at once, and it felt like her pain had no end. “I felt responsible for his suffering,” she said.
Famodun had initially hoped that her son would reach developmental milestones like walking, sitting, and talking, just like other children. However, she later learned from the doctor at LUTH that the recovery process takes time and is quite unpredictable.
After her supervisor at work learned about her situation, she was granted a one-year paid leave. This period allowed her sufficient time to recover from the emotional turmoil and adapt to her new role as a caregiver.
Her husband helped her through this life transition. “My husband offered counsel on several occasions and taught me how to efficiently manage my time, ensuring I could care for Tiolu before leaving for work,” she shared.
However, as she grew stronger in her role, her husband’s support waned. Four years later, he lost his contract job and eventually stopped returning home, choosing instead to live in the church for the next few months.
Feeling abandoned, Famodun slipped back into depression. She was now left alone to cater for the family’s well-being while shouldering Tiolu’s medical expenses.
Famodun’s list of creditors was steadily growing. She had resorted to borrowing money to cover her transportation costs to work and purchase Tiolu’s medications, which cost well above 50,000 naira ($50) monthly. The financial strain became so severe that she switched Tiolu from diapers to cloth napkins to reduce expenses.
Regardless of the challenges she faced, Famodun remained kind and friendly in her interactions with people. However, she wished that people were more open to children like Tiolu.
One day, during her commute to work on a public bus, she sat beside a woman who seemed visibly uncomfortable around her son because he was drooling. The woman made concerted efforts to maintain some distance between Famodun and her child. This woman’s behaviour might have been influenced by a prevailing myth that contact with bodily secretions from children like Tiolu could lead to contracting the condition.
Sadly, such incidents were not uncommon. Every time Famodun went out with her son, she also had to deal with unfriendly strangers.
This has made socialising an arduous task for the friendly Famodun, who increasingly feels her son is not wanted by society.
Consequently, she started declining party invitations, opting instead to spend her time with Tiolu at home.
A Common Trend
Negative social life is often reported by parents and caregivers of children with neurodevelopmental disorders.
Rosemary Odileke, a 41-year-old mother of two autistic children, noticed a significant change in her relationships after their birth. Her friends distanced themselves, and she received fewer party invitations. “At some point, we stopped receiving invitations,” she said.
“To be honest, this change might actually be for the best,” she admitted, “when we go to parties, I hardly get to relax. I have to constantly keep an eye on my children to ensure they don’t damage anything,” she added.
Odileke acknowledged that her children’s invisible disability makes it challenging to garner sympathy from strangers. “Because there are no visible physical disabilities, people tend to assume that my children are simply badly behaved.”
According to Lillian Akuma, a physiotherapist at the Child and Adolescent Centre of the FNPH, “Autism is a group of complex disorders characterised by difficulties in social interaction, repetitive behaviour, sensory disorders, and verbal and non-verbal communication.”
A devout catholic, Odileke shared that her children’s condition strengthened her faith in God, and she ensured to attend all the church’s activities.
At a much anticipated cultural event at her parish, while Odileke was searching for a suitable seating spot for her family of five, she overheard a woman whispering to another, “See those children that act like mad people.” The woman’s gaze was fixed on Odileke’s children.
Though she felt deeply embarrassed, Odileke remained silent, not wanting to spoil what was supposed to be an exciting day at church for her family. However, tears welled up in her eyes, forcing her to go to the restroom before anyone could notice she was crying.

In 2018, when she received the diagnosis of autism for her two kids, she recalled feeling demoralised, especially upon learning that there was no cure for the condition.
“Sometimes, I feel overwhelmed, as if the world is ending,” she said.
If the children become restless, she would take them for long walks in the hope of wearing them out. Ironically, she often ends up more exhausted herself.
“Most times, the stress triggers migraines,” she said. While she has been prescribed medications to manage the debilitating headaches, they aren’t always effective “because the primary trigger is still present.”
“In this state, I’m unable to care for my children. But when I look around, there’s no one to call,” she said.
Previously, Odileke’s niece provided support in caring for the children, but she left after gaining admission to a higher institution in Edo State, which was a six-hour journey from Lagos, where Odileke and her family live.
As her work demands grew, Odileke was compelled to hire a nanny to look after the kids until her return in the evening, paying the nanny 20,000 naira ($14.7) monthly. At one point, she even hired a physiotherapist to provide additional therapy for the children but struggled to pay the monthly wage of 40,000 naira ($30).
The Cost of Care
In the UK, the government provides two social security benefits systems for children who have disabilities: the Disability Living Allowance (DLA) for children under 16 and the Personal Independence Payment (PIP) for older teenagers above 16. The allowance provided varies from £26.90 (43,000 naira) to over £101.75 (162,800 naira) per week, depending on the level of assistance the child requires.
However, the situation is different in developing countries like Nigeria. The national law to protect the rights of persons with disabilities (PWDs), the Discrimination Against Persons with Disability (Prohibition) Act of 2018, lacks specific provisions for allowances for children with disabilities.
According to the Nigerian researcher Olagunju and his colleagues, “Caregivers in resource-restricted countries do not only play a central role in ensuring the well-being of these children but are sometimes solely saddled with significant treatment responsibilities.”
He attributed it to the unequal distribution of treatment resources, high out-of-pocket expenses, and limited health insurance coverage in these countries.
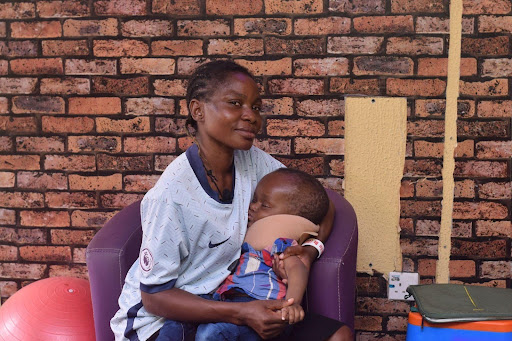
Stella Igbokwe, a young mother whose only child was diagnosed with hydrocephalus, a condition in which excess cerebrospinal fluid builds up within the fluid-containing cavities or ventricles of the brain, disclosed that she spends more money on her child’s care than she earns from selling fruits on the street.
“I spend over 50,000 naira ($37) every month on my son, Stanley. It costs 20,000 ($14.7) naira to register him at Flora’s Trust Centre. The remaining amount covers his medications, diapers, special diet and transportation; it is not easy,” she lamented.
Flora’s Trust Centre, a private formal caregiving home, was founded by Chikaodili Ugochukwu, a 55-year-old mother of a teenage son living with cerebral palsy.
When Ugochukwu began the centre in 2018, it was exclusively dedicated to children living with cerebral palsy, but it was impossible for her to turn her back on mothers raising children with other neurological disorders “Disability management is a herculean task,” she said.
Recognising Igbokwe’s plight, Ugochukwu felt obligated to take in her son to ease the burden on the young mother who receives no support from her partner.
“Once I drop him off at the centre, I feel a sense of relief, knowing I can focus on my work. My primary concern now is ensuring that I have enough money to pay for another month,” Igbokwe said.
Although there have been instances where children were admitted without the enrollment fee, Ugochukwu soon found that this practice was not sustainable.
“We are non-profit, but in the meantime, we require parents to pay subsidised fees to cover our operational expenses until we can attract more sponsors,” she explained.
Ugochukwu revealed that it costs no less than 800,000 naira ($590) to keep the centre running. This covers their overhead cost and enables them to employ the services of professionals to offer physiotherapy, speech and occupational therapy for the children.
On the centre’s two-tone wall, a whiteboard displayed the names of enrolled children. There were 11 names, although only five children were present at the time of this report.
Among the absentees was Ifedayo*, a 12-year-old girl living with cerebral palsy. Her mother, Ayomide*, a 49-year-old single parent, had not renewed tuition for that month because Ifedayo’s older brother was on holiday and would be supporting her at home.
When her husband was alive, Ayomide never considered caregiving centres because he effectively supported her at home, even at some point becoming Ifedayo’s primary caregiver.
“After my husband passed away, I was really under pressure,” said Ayomide, who became the sole breadwinner of the family.
She said that it was impossible to make ends meet while providing round-the-clock care for her daughter. “I was struggling to meet deadlines at work, and not all my clients were understanding.”
She stumbled upon Flora’s Trust Centre by chance and decided to enrol in Ifedayo after learning about the centre’s weekly boarding services. This meant parents could drop off their children on Monday mornings and pick them up at the end of the week.
Even after she found that this would cost her 60,000 naira ($44.2)—significantly higher than the centre’s non-boarding services—she still went ahead with her decision.
“It’s not that I could afford the money, but commuting daily to the centre would cost almost double the amount,” she explained, referring to the mobility challenges she experiences when going out with her daughter, whose condition confines her to a wheelchair.
False Hope
At first, Ayomide had thought that diligently following her daughter’s treatment plan would help her recover. “But there seems to be no end,” she said.
Like those who came before her, she would realise that caring for children with special needs is a journey, not a sprint.
“Many of these children will rely on their parents throughout their lives,” said Akuma, a physiotherapist with over 12 years of experience working with children and adolescents living with neurological disorders.
“What I often observe is that many caregivers are unprepared for the transition from childhood to adolescence and eventually adulthood,” she continued. She noted that health professionals who provide care for these children were partly to blame.
“In a bid to comfort parents, we give them the impression that it’s just a phase the child will outgrow. But that’s not always the case,” she explained.
These parents, clinging to this prognosis, become anxious to witness their children reach important milestones. “They hope to see their children stand, but after two years, if the children haven’t even achieved neck control, the parents become depressed,” she said.
“I have conducted research on caregiver’s burden and discovered that when they are in this mental state, they no longer put in their all to support their children,” Akuma said.
“When caregivers fail to fulfil their roles effectively, we can’t expect positive treatment outcomes for the children,” she concluded.
A Safe Place
The FNPH’s annexe, The Child and Adolescent Centre, also located in Lagos, is one of the few facilities offering medications for children with neurological disorders.
However, it holds a significance far beyond being just a healthcare institution for many of these mothers.
“The Child and Adolescent Centre is like a family house for me,” said Wemimo Akinwunmi, a 39-year-old mother of a son living with cerebral palsy. Her son, Ayomikun, had earned the endearing nickname “Ambode” from fellow parents at the centre, which was a nod to a former governor of Lagos State whose first name was also Akinwunmi.
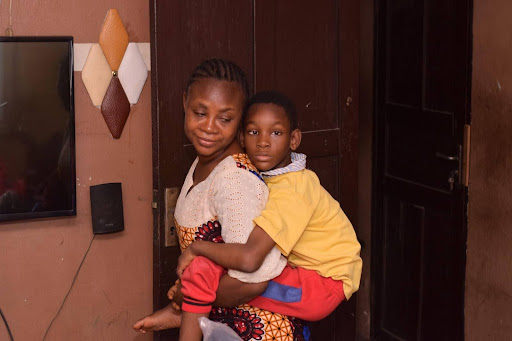
Akinwunmi recounted when she ran out of money for her son’s medication and the other parents rallied to provide the outstanding amount. On days when she had enough, she returned the favour to other parents in need.
The centre has gained immense popularity for two key reasons: first, its specialised treatment for children with neurological disorders, and second, as a safe space where their parents feel genuinely understood.
Famodun disclosed that the centre played an important role in restoring her confidence. ‘In 2016, I was transferred to the pharmacy section of the Children and Adolescent Center, where I met numerous mothers who shared similar experiences. I learned so much from them,” she said. She also benefitted from the return of her husband, whom she described as supportive.
These days, when parents visit the clinic, the nurses frequently turn to Famodun to address their concerns. “I went from being quiet to becoming an activist for my son,” she said, smiling proudly.
Good Laws on Paper
Among the eight Nigerian states acknowledged in an Office of the High Commissioner for Human Rights (OHCHR) report for incorporating regional disability laws, only five allocated a portion of their 2023 budget to support the law’s implementation. Lagos State, the focal point of this report, stands out. Notably, the Lagos State Disability Fund, dedicated to enforcing Lagos State Special People’s Law (LSSPL), surpassed the combined funds of the other four states.
The women in this report expressed a need for effective social support programmes and government policies to ease the burden of caring for their children’s education and healthcare needs. But none of the women in this report were aware of LSSPL, which was enacted in 2011 for this purpose, even though they all reside and work in Lagos State. In fact, they doubted its existence, having never heard of anyone benefiting from its provisions.
According to the legislation, children living with disabilities are entitled to “free and continual medical treatment in any public health institution.” However, it is a different picture in reality as access to free healthcare remains an unfulfilled promise for Persons with Disabilities (PWDs) in Lagos, a fact highlighted in a 2020 report by the Centre for Citizens with Disability (CCD).
The report revealed that inadequate funding and the absence of specific policy guidelines impede the ability of the state’s Ministry of Health to provide free healthcare services to PWDs.
Regarding education, the LSSPL mandates free tuition at all levels in public institutions. Currently, Lagos has 50 public special needs schools—five non-inclusive special needs schools and 45 inclusive ones—but the few mothers who attempted to enrol their children in these schools were met with profound disappointment due to the bad condition of the facilities and understaffing.
Akinwunmi recalled her husband’s visit to a nearby special needs school after someone she met on her street recommended it. After his visit, he dismissed it as an option due to the poor condition of the building and insufficient teachers, noting just two teachers for the large number of special needs children he saw running around the school facility.

While there is no global standard for the teacher-to-student ratio, Nigeria’s National Policy on Education suggests a ratio of 1:40. The national average in basic education schools, as per the 2022 Universal Education Basic Commission (UBEC) annual report, stands at 1:28, well within this benchmark.
Nevertheless, in Lagos State, the National Bureau of Statistics indicates a higher ratio of 1:50. A 2020 report by three disability rights organisations, including the Lagos State Chapter of the Joint National Association of Persons with Disabilities (JONAPWD), found that 44 inclusive schools across Lagos State’s six education districts showed inconsistencies in the distribution of special teachers. In certain districts, the ratio was as high as 1:75, which was considered inappropriate as children with disabilities require additional attention and resources to facilitate learning.
The LSSPL has suffered from inadequate implementation, and earlier in 2023, the Lagos State Office of Disability Affairs (LASODA), the body responsible for implementing the law and managing its finances, was accused of misappropriating funds by its members.
Following the accusation, the general manager of LASODA, Dare Dairo, absolved his office of any wrongdoing, emphasising that they lack the authority to withhold funds. He noted that they were working in collaboration with local government officials to enhance healthcare access and inclusive education for PWDs.
In April 2023, Dr Adebukola Adebayo, Chairman of the state’s JONAPWD, urged the state governor to establish a panel to investigate LASODA’s financial activities and projects. In the news article published on BONews, Adebayo explained the reasons behind his demand, stating, “[An] independent audit of the agency and its managers will expose fraud and corruption in the execution of projects and non-compliance with the Lagos State Procurement law.”
To give LASODA a right of reply in seeking clarification on how the agency disbursed the state government funds to achieve the diverse objectives of the LSSPL, I reached out for clarification.
Dairo did not respond to my inquiries and requests. On October 24, 2023, I submitted a written request at the LASODA office in Alausa, Lagos State, in accordance with the guidelines of Nigeria’s Freedom of Information Act. However, neither Dairo nor a representative of LASODA provided a response.
It is important to note that while Dairo was the General Manager of LASODA at the time of producing this report, he has since been replaced. Adenike Oyetunde-Lawal assumed the office on December 19, 2023.
Tobiloba Ajayi, a lawyer living with cerebral palsy who played a role in developing the LSSPL, expressed her frustration. “The law covers everything. It was beautifully written. We put in all the work to get the law passed, and yet, here we are,” she said.
“It has been 13 years, and implementation has continued to be lacking,” she stated.
Ajayi criticised the government’s patronising attitude towards PWDs as the main reason behind the slow implementation of the law.
“As long as the people who are supposed to implement these laws still think they are doing people living with disabilities [PwDs] a favour, we will achieve nothing,” she concluded.
*Some names have been changed to protect their identities.
*Chikaodili Ugochukwu lost her teenage son some months after this interview was conducted.
*Exchange rates used were based on the time of report
This story was produced with the support of the Women Radio Centre and the MacArthur Foundation.
Support Our Journalism
There are millions of ordinary people affected by conflict in Africa whose stories are missing in the mainstream media. HumAngle is determined to tell those challenging and under-reported stories, hoping that the people impacted by these conflicts will find the safety and security they deserve.
To ensure that we continue to provide public service coverage, we have a small favour to ask you. We want you to be part of our journalistic endeavour by contributing a token to us.
Your donation will further promote a robust, free, and independent media.
Donate HereStay Closer To The Stories That Matter




