Mobile Clinics Providing Aid To Inaccessible Communities In Northeast Nigeria
Mobile clinics supported by aid organisations are providing medical assistance to communities in hard-to-reach areas of Borno, Adamawa, and Yobe states that are affected by the decade-long insurgency.

The decade-long insecurity crisis in the Northeast of Nigeria leading to displacements and other forms of humanitarian adversities have rendered many sections of Borno, Adamawa, and Yobe States hard to reach.
This has exposed thousands of residents and internally displaced persons (IDPs) to a myriad of diseases such as cholera, tuberculosis, and malaria.
A recent finding from an assessment of 17 Local Government Areas (LGAs) in Adamawa and Borno states revealed that barriers to accessing healthcare services were reported in up to 95 per cent of the communities evaluated, while 11 per cent had healthcare facilities destroyed due to the ongoing insurgency.
But there has been a relief as mobile clinics of about 113 medical and health personnel are taking health care delivery to the hard to reach communities.
The medical teams consisting of professional nurses and midwives, community health workers, and health record assistants equipped with medical kits are providing essential basic health care to the hard to reach places in the three hard hit states of Borno, Adamawa, and Yobe.
They provide services such as coordinating surveillance, outbreak prevention of endemic diseases including treatment for malaria, pneumonia, and sexually transmitted infections in 2,300 hard to reach communities.
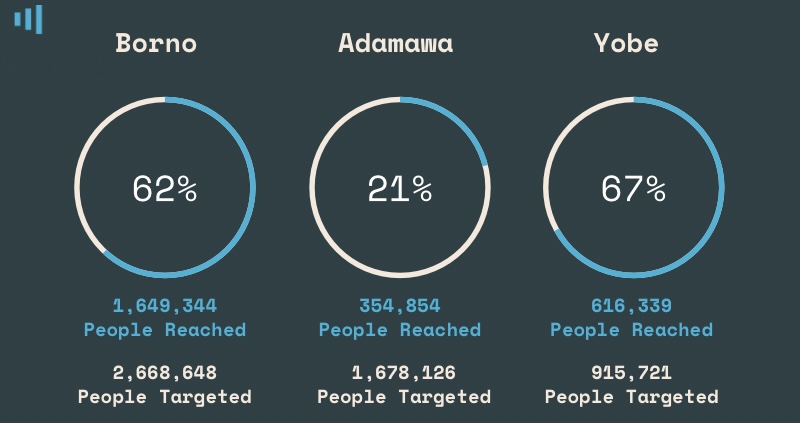
According to the Health Sector Humanitarian Response Dashboard from Jan. to Dec. 2021, over 2.6 million people were reached in these three states. They were IDPs, returnees, and members of host communities.
The data indicates that more women than men were beneficiaries of primary health services with the average age bracket being from 17 -59.
Brains behind mobile clinic
The World Health Organisation (WHO), Health Sector Partners, and other UN agencies are facilitating the mobile clinics to inaccessible and underserved communities.
Fatima, one of the beneficiaries of the medical intervention provided by the mobile clinic was treated for severe malnutrition. Hadiza, her mother revealed Fatima was diagnosed with the condition and was referred by the team to Wawa Primary Health Care centre in the outskirt of Borno State.
Fatima’s case led to a referral to a stabilisation centre for in-patient management of severe malnutrition with medical complications in Umaru Shehu Stabilisation center, in Maiduguri, the capital of Borno.
“Her medical condition needed to be stable first so that we can handle her nutritional rehabilitation. All efforts proved worthy as Fatima’s case improved tremendously within one month of treatment,” said Mrs Musa, one of the team members.
Access to healthcare outside hard-to-reach areas
According to WHO, access to healthcare facilities entails the availability of competent and skilled health workers, accessibility taking into account demographic composition, acceptability from health workers to treat all patients with dignity while establishing trust; and quality of health workforce.
In Nigeria, the patient to doctor ratio is currently at four doctors to 10,000 patients. Which is far from the WHO’s recommendation of the 1:600 standard. This has been linked to the emigration of medical practitioners to foreign countries due to a lack of work tools, poor working conditions, and insecurity as revealed by Innocent Ujah, President of the Nigerian Medical Association.
Ujah lamented that over 50 per cent of Nigerian doctors are outside the country. “We estimate that about 80,000 Nigerians have been trained as doctors but only about 40,000 are at home.”
Majority of vulnerable and displaced communities across Nigeria rely on humanitarian assistance and medical support from Aid organisations.
The global health body predicts that by 2030, 60 million lives can be saved in low and middle-income countries, and life expectancy can improve by 3.7 years if primary health care interventions are scaled up.
Support Our Journalism
There are millions of ordinary people affected by conflict in Africa whose stories are missing in the mainstream media. HumAngle is determined to tell those challenging and under-reported stories, hoping that the people impacted by these conflicts will find the safety and security they deserve.
To ensure that we continue to provide public service coverage, we have a small favour to ask you. We want you to be part of our journalistic endeavour by contributing a token to us.
Your donation will further promote a robust, free, and independent media.
Donate HereStay Closer To The Stories That Matter




