Drones Are Delivering Medical Supplies To Hard-To-Reach Clinics In Nigeria
Where medicines could take hours to reach, a logistics company is maximising drones to get them to Primary Healthcare Centres across some cities in Nigeria. We took a look at their operations in Kaduna State.

Rebecca John went into labour in the dead of night.
This was not supposed to be unusual at facilities like Kari Kunau Primary Health Centre. But Idris Isah, the In-Charge, was worried. Theirs was a small clinic in a remote part of Lere local government area of Kaduna State, Northwest Nigeria. They could hardly store any medical product that needed refrigeration.
Now his patient, Rebecca, had suffered some complications – she urgently needed a blood transfusion. And their centre was usually not allowed to give blood transfusions, he said. “But this was an emergency.”
This event took place in the month of Feb. 2023. An experience Isah would always remember.
So, they made an order by phone for pints of blood from a logistics company. “Sometimes we send text messages or use Telegram. But this was different. They knew who we were and our location the moment we called because they have our contacts,” Isah explained.
Saved
Within five to ten minutes, a drone sliced through the night and dropped a package by Kari PHC. Isah and his assistants rushed to set up a line for Rebecca. In the end, “she delivered successfully and we referred her to a general hospital,” he told HumAngle.
Kilometres away in Kauru, Wada Yunusa, who is the In-charge of Ibada Primary Health Clinic said it had been a herculean task accessing medical care for a while. When patients leave the facility, it is usually with a drug prescription that even he knows may be impossible for them to get nearby.
“They go in search of the drugs and sometimes they don’t get them in pharmacies. They go as far as Pambegua or even Zaria before they get them,” he said.
One of Yunusa’s patients, Lawal Hassan, recalled how he suffered from an illness for three weeks. Unfortunately for him, he was being prescribed medication that proved ineffective.
“I was experiencing dizziness and pain around my chest…weakness and fever. The drugs I was getting were not working until the clinic ordered from Zipline.”
Hassan is not alone. James Jacob walked into Nasaru Primary Health Clinic early one morning when this reporter visited. He needed to access drugs supplied by Zipline in the facility located in Hayin Gada, a settlement in Kubau LGA of Kaduna State.
“I suffered from ulcer and it was the drug ordered that day that helped me,” he said, referring to the logistics company. And now, before travelling out of Hayin Gada to Kaduna, he was bent on getting some medication directly from the same source. This is also because the organisation does not supply to individuals and it had to be through a PHC.
In 2022, the National Primary Healthcare Development Agency (NPHCDA) said that over 70 per cent of medicines distributed in Nigeria were substandard. It also pointed out that the “majority of Nigerians do not have access to health services; 20 per cent of all maternal deaths globally occur in Nigeria; infant mortality occurs at a rate of 19 deaths per 1,000 births. Children under five are dying at a rate of 128 per 1,000, while over 70 per cent of medical drugs dispensed in Nigeria are substandard.”
The report further added that the weakness of the PHC system in the country made it become under-utilised and a burden to the health sector “with patients over-lying on tertiary and secondary health care services.”
Another report described Nigeria as the most counterfeit market in the developing world. Before then, another by Punch focused on “how fake drugs threaten Nigeria’s multi-billion pharma industry.”
Meanwhile, the National Agency for Food and Drug Administration and Control (NAFDAC) continues to destroy fake drugs worth hundreds of millions across the country. In January this year, its Director General, Prof. Mojisola Adeyeye said the agency has spent over $2,4 million on purchasing scanning machines to test the standard and quantity of drugs in Nigeria. All these paint a disheartening picture about Nigeria’s Primary Healthcare system.
Hit and run
They were losing blood. So much blood.
One man had a head injury that badly needed stitching. The other was bleeding from a deep cut in his leg.
Both cases needed urgent attention.

Just minutes ago, the two would-be patients were speeding towards Pambegua on a motorcycle. It was drizzling when a vehicle hit them, shoving them off the road.
They stood no chance – their motorcycle skidded off the road and crashed.
Fortunately, passers-by who had witnessed the incident came to their rescue. The two men were rushed to the nearest healthcare facility – Nasaru Primary Health Clinic, located in Hayin Gada, a settlement in Kubau Local Government Area (LGA) of Kaduna State, Northwest Nigeria.
It was hard to believe that just a little while ago, Auwal Shatiu, 33, and Aniru Umar, 26, had been the riders of a speeding bike. They had been eager to take advantage of the weekly Friday market in Pambegua that day of Sept. 16, 2022.
Now they were both bleeding profusely.
At the clinic, Abdulazeez Tanimu, a Routine Immunisation (IR) officer, and his team that included a volunteer and two interns knew what to do. Or, at least, Tanimu did. There was no one else to save Shatiu and Umar’s lives. This rural clinic does not have a single trained doctor.
Although an RI officer saddled with immunisation responsibilities every other Thursday, Tanimu was confident. He knew this – “In road traffic accidents there’s usually a need for stitching, dressing and then some drugs,” he told HumAngle.
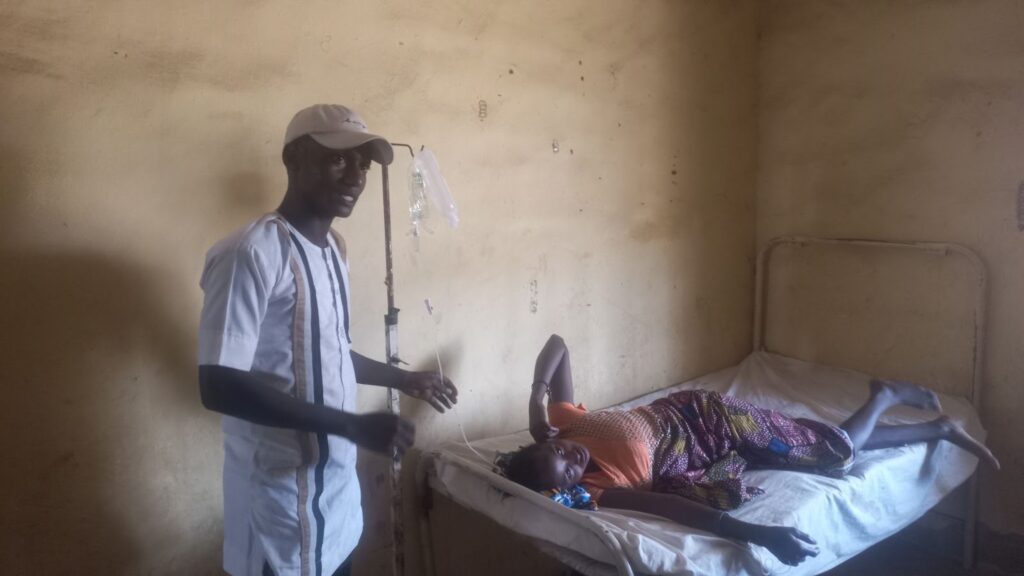
Tanimu moved into action and called Zipline. In less than fifteen minutes, a drone flew over the small clinic at high speed. A parachute snapped open and, with yelling children rushing towards it, a package landed just by the building. On a red box, the word Zipline was written boldly.
The RI officer was expecting it. The logistics company had a system in place which communicated when a delivery was five minutes and then two minutes away.
He tore the package open – inside were drugs, including anti-tetanus injection, some cotton wool, bandages, plaster, and medicine for the IV line they would set up.
Help had come just in time. But at a price – Everything cost about ₦9,000 ($19.53).
Komla Buami, the company’s Director of Communications Africa, told HumAngle that from the Pambegua centre, Zipline has the capacity to make flight runs that average between 150 to 250 per day.
This reporter witnessed three launches in about 10 minutes at Pambegua. If Zipline makes 200 launches at an average of N9000, that would be ₦1.8 million in a day and roughly ₦657 million per year.
Currently, the organisation has a staff strength of over 50 persons at the Pambegua centre.
“All our staff are industry experts in various fields, including pharmacy, engineering, biochemistry, medicine and other skills as the job requires,” Buami said, adding that he could not disclose their salary range or the company’s yearly cost and turnover. “All installations, including all capex and opex, at all our operational centres are funded by Zipline just like any other private company.
Buami explained further that the logistics company is “a wholly private-owned company in a public-private partnership with the Kaduna State Government.” It has an American, Keller Rinaudo Clifton, as its co-founder and CEO.
As a result of this partnership, the organisation receives medical commodities and blood products. These they deliver on behalf of the state government to identified health facilities within the state. The government then pays the delivery cost as agreed between the parties.
The drones
A little while back, the flight operations team at Zipline headed by Jeremiah Dunah had received Nasaru Health Clinic’s order by phone in their Pambegua office, also in Kubau LGA. And, like Tanimu, they too had moved into action. Their role, they knew, was important. What would take a vehicle thirty minutes, an hour or three, took their drones ten or thirty minutes.
The team usually split their deliveries into categories, Dunah explained. There is that of replenishments when a medical facility is running low on medical products and the company ensures they are stocked as and when due. A typical example are vaccines.
Then there are also scheduled deliveries, when, for instance, a hospital needs to carry out a surgical operation and would need a particular product. “They call and let us know when they need it and we deliver. We schedule such deliveries,” Dunah said.
For emergencies, like when a woman is in labour and a particular medication or blood type is needed, they swing into action. A part of the team they call fulfilment operators from the warehouse to prepare the order, package it and hand it over to the flight operators.
Now, the Nasaru Clinic’s order was an emergency. This puts it under the most important category.
But there was something else.
The logistics company has a strategy called facility mapping. This is when they get the coordinates of all PHCs within their area of operations. After that they do facility onboarding where their community leads ensure they record each clinic’s needs at different times.
Such an approach automatically meant the organisation and PHCs had already established a relationship. In this way, the facilities could easily reach out to them and they in turn have their coordinates and could deliver as swiftly as possible.
“It has four different components,” Dunah explained about the drone. “It has the musicum, the wing, the body, and the battery to power it. The drone can travel for three hours and moves at a speed of 110 metres per second.”

He added that it can fly from Pambegua, Zipline’s current base in Kaduna State, to its capital and return in under forty minutes. This is usually a two-hour (one-way) trip by road.
“It can also carry a package that weighs up to 1.75 kg.”
To access the flight area, one passes through a room where the drone batteries are charged. The battery, apart from powering the drone, also has a memory card that helps the team save the flight log. In this way, they get feedback on the weather condition. There is also a GPS antenna on it that communicates the drone’s location.
“So, we always know where the drone is, including its altitude,” Dunah said. “Apart from the antenna on the battery, we have another on the body of the drone. Their purpose is to check each other and ensure that they communicate the same location. If there’s a discrepancy in their communication the drone calls it mission failure and returns to base. The drone always knows how to come back home.”
In the flight area, a flight operator puts the drone on the launcher, before a runway that is actually a slanted platform facing skywards. Then an electronic voice from a device announces the flight schedule. The operator hits a button and the drone takes off.
It was not until later that the flight team knew that that particular vital delivery to the clinic in Hayin Gada helped to treat accident victims.
Supply chains
One of the United Nation’s third Sustainable Development Goals (SDGs) includes access to safe, effective, quality, and affordable essential medicines and vaccines, for all.
A Jan. 5, 2022 research work published by BMC Public Health focused on the challenges associated with medicines and vaccines supply chain systems in Nigeria. Their findings show that there are several challenges that include difficulty with medicines or vaccines selection, procurement, distribution, and inventory management.
There is also poor storage infrastructure as is the case with PHCs across Kaduna State and Nigeria in general. At the moment, Zipline serves up to 500 facilities that lack the capacity to store vaccines within the state, including Nasaru Health Clinic.
“Vaccines such as that of Yellow Fever, measles and many more require a certain cold temperature in order to preserve them. It doesn’t like heat. If the temperature is too high, the vaccines would lose their potency,” Khalid Tasiu, the in-charge of the clinic, told HumAngle. What’s worse, the facility itself lacks access to electricity supply.

Zipline, on the other hand, has a warehouse with about five refrigerators for cold tin products. “These are products to be stored in cold temperatures,” Rukayya Abdulsalam, the Fulfilment Operator, said. “For some of them, it’s between two to eight degrees centigrade while some are frozen below zero degrees centigrade.” These include vaccines, blood, and other medical products.

Others are stored on shelves in the warehouse – they are kept under room temperature of about 16 to 26 degrees centigrade. Six air conditioners make this possible while a device checks the temperature to ensure it remains accurate. These are facilities many PHCS cannot boast of across the country.
The logistics company gets their medical products from the Kaduna State Health Supplies Management Agency (KADCHMA), Rukayya said. To ensure they are in good condition, they, after procurement, conduct visual inspections where they ensure the drugs are not broken or leaking. They also look out for expiry dates and batch numbers.
When the supplies are certified as safe, they are delivered to only the facilities within the Pambegua office service radius – “which is from eighty to ninety kilometres,” she said, adding that the organisation is working at building another base around Kafanchan in its bid to expand operations across the state. Already, it has operations in Bayelsa and Rivers State.

Mission failure
Sometimes the drones do not complete their mission, HumAngle gathered.
“We don’t just fly,” Dunah said. “It’s an airspace and there’s a regulatory body that we always communicate with. Before launching every drone, we have a system we call the bird watch, which enables us to communicate with the regulatory body. Just like airports have a controller, we also have our in-house controller. We always communicate, with the controller, regulatory body and the airport.”
In cases where there are other unmanned aircraft in the air, the flight operations team at Zipline would spot it on their system. In such a situation, they either call back their drone or put it on temporary hold – it flies in circles until the other aircraft passes. This usually causes some delay in delivery of between three to five minutes.
Another challenge is when it gets windy. Although the drone is built to withstand any type of weather, whether rainy or sunny, there are peculiar cases.
“We don’t fly when there is high wind because it takes the drone out of the flight path. We don’t have a system on the ground to tell us when the wind is changing.”
There are other instances where the drone gets to the facility it is supposed to deliver to and high wind affects accurate delivery. This is when it declares mission failure and returns to base.
Another challenge is when the company sends a drone to a place that lacks network coverage. On such an occasion, the flight team waits patiently until it returns before they can ascertain the time it fulfilled its mission.
Once, Khalid Tasiu, the in-charge of Nasaru Health Clinic and Tanimu, the IR officer had a dicey situation on their hands. They had a boy patient who was suffering from Sickle Cell Anemia. He needed blood and they quickly made an emergency order. But Zipline said it did not have that particular blood type and the clinic had to look elsewhere.
Rukayya, the organisation’s Fulfilment Operator recalled how insecurity and bad roads affect access to certain locations. A typical example is the PHC at Galadimawa in Lere local government area.
“We support them, particularly by providing routine immunisation vaccines they do for children every Monday. Before Zipline came, they had challenges getting the vaccines,” she said.
“Now we are able to send the vaccines to them in good condition. The vaccines are supposed to be kept in a cold chain, and before they were able to get them in the past, it could be difficult and the ice might melt. So we are able to send to them and they don’t have to order from very far locations in a place where they could get attacked due to insecurity.”
Summary not available.
Support Our Journalism
There are millions of ordinary people affected by conflict in Africa whose stories are missing in the mainstream media. HumAngle is determined to tell those challenging and under-reported stories, hoping that the people impacted by these conflicts will find the safety and security they deserve.
To ensure that we continue to provide public service coverage, we have a small favour to ask you. We want you to be part of our journalistic endeavour by contributing a token to us.
Your donation will further promote a robust, free, and independent media.
Donate HereStay Closer To The Stories That Matter




